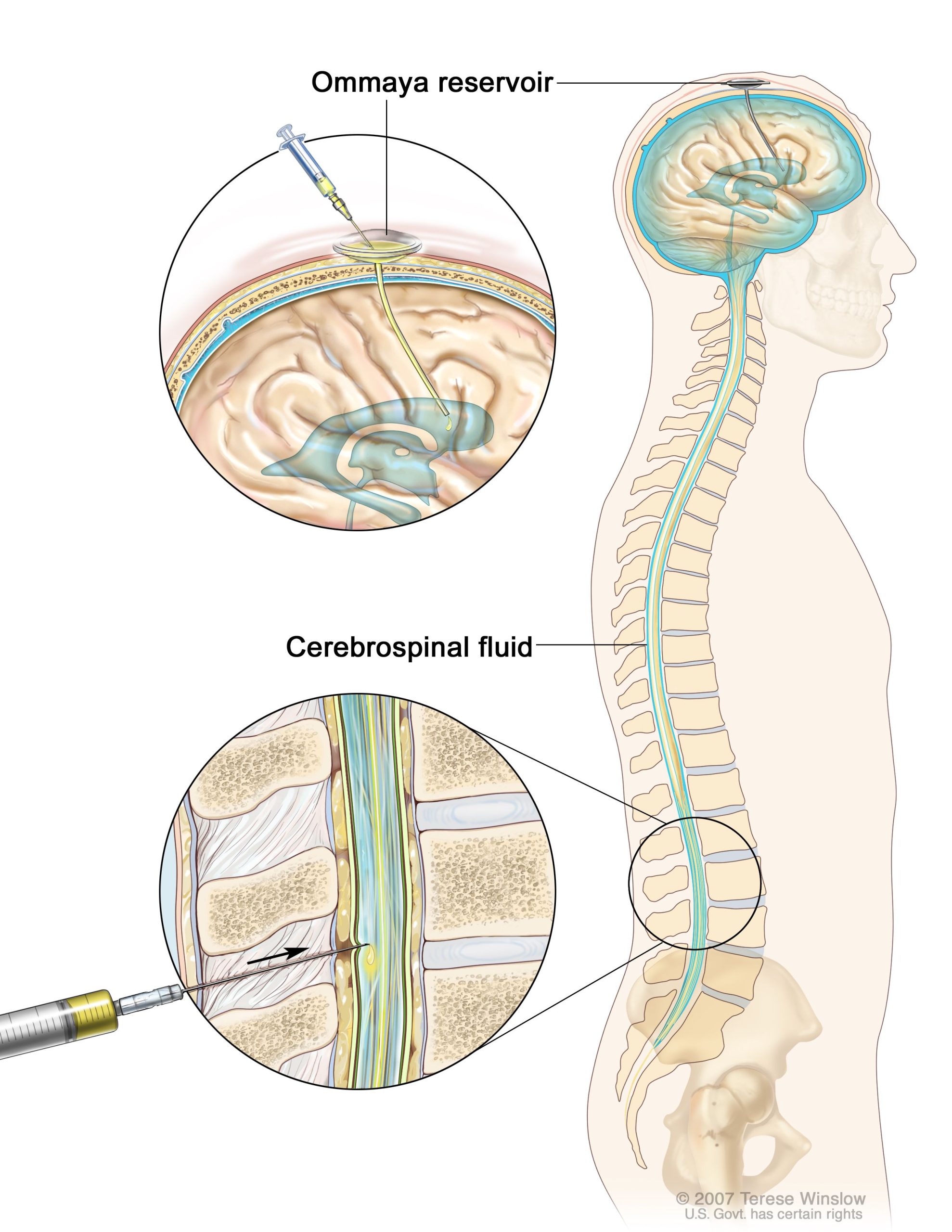
Intrathecal Chemotherapy Methods
Intrathecal chemotherapy delivers drugs directly into the cerebrospinal fluid (CSF), targeting cancers within the central nervous system (CNS). This localized approach ensures higher drug concentration in affected areas, bypassing the blood-brain barrier. Neurologists and oncologists use this technique to treat various CNS cancers. The precision of intrathecal chemotherapy highlights advances in medical procedures, offering hope for many patients battling complex neurological malignancies. Recognizing its significance empowers patients and caregivers in the fight against challenging CNS cancer conditions.
Overview of Intrathecal Chemotherapy
What Makes Intrathecal Delivery Unique?
Intrathecal delivery allows direct access to the CNS, overcoming the limitations of systemic chemotherapy. This method bypasses the protective blood-brain barrier, which often prevents adequate drug penetration. Administering treatment in this way targets malignancies more accurately, minimizing systemic exposure and reducing potential side effects. Physicians prefer intrathecal routes when localized CNS delivery is crucial, ensuring effective treatment while sparing healthy bodily systems from unnecessary chemical exposure.
How Chemotherapy Reaches the CNS
Chemotherapy drugs are introduced into the CSF, where they can diffuse throughout the CNS. This approach targets brain and spinal cord tumors more effectively than systemic options. By directly bathing the affected areas in potent oncological agents, intrathecal chemotherapy ensures high drug concentrations. This method enhances the direct impact on malignant cells, is crucial for conditions resistant to other dosage forms, and optimizes therapeutic outcomes for patients with CNS involvement.
When and Why It’s Prescribed
Oncologists prescribe intrathecal chemotherapy for tumors affecting the CNS or leptomeningeal spread of systemic cancer. Its specificity allows for concentrated treatment directly at the disease site. This targeted approach is particularly suitable for patients for whom other chemotherapy forms are ineffective or insufficient. Physicians choose intrathecal delivery to maximize cancer drug efficacy, ensuring therapeutic interventions are both potent and precise, often as part of a broader treatment plan.
Methods of Administration
Lumbar Puncture Technique
The lumbar puncture technique involves inserting a needle into the lower back’s subarachnoid space, allowing drug administration directly into the CSF. This procedure is performed by skilled healthcare professionals in a controlled environment to ensure patient safety. It is a common method for delivering intrathecal chemotherapy, offering direct access to the CNS. Patients are closely monitored during and after administration to mitigate potential complications and ensure optimal treatment delivery.
Ommaya Reservoir Method
An Ommaya reservoir is a surgically implanted, dome-shaped device beneath the scalp. It provides repeated, easy access to the CSF for drug administration without multiple lumbar punctures. The reservoir connects to the lateral ventricle of the brain via a catheter, enabling precise delivery of chemotherapy. This method minimizes patient discomfort and supports regular monitoring and cerebrospinal fluid sampling, proving beneficial for long-term treatment regimens.
Catheter-Based Delivery Systems
Catheter-based systems involve placing a catheter surgically into the CSF space, such as the intraventricular or lumbar regions. This method facilitates continuous or intermittent drug infusion, tailored to treatment requirements. Catheter-based delivery offers flexibility in managing dosing schedules and reduces discomfort compared to repeated needle punctures. It is utilized in patients requiring frequent or prolonged therapy, optimally balancing efficacy and comfort.
Treatment Protocols
Dosing Schedules and Drug Cycles
Intrathecal chemotherapy protocols specify dosing schedules and cycles based on the cancer type and patient response. Physicians determine drug selection and frequency, ensuring adequate tumor exposure while minimizing toxicity. Treatment regimens might vary from weekly to monthly administration, adjusted as necessary. Regular monitoring allows oncologists to tailor therapy intensity, optimizing patient outcomes through precise, individualized treatment plans.
Combination with Systemic Chemotherapy
Intrathecal chemotherapy is often combined with systemic chemotherapy to enhance therapeutic efficacy. This dual approach targets malignancies both within and outside the CNS, tackling cancer from multiple fronts. Oncologists tailor these combinations based on the tumor type, patient health, and treatment goals. Combining treatment modalities increases comprehensive cancer management, offering patients an integrated strategy for combating complex diseases.
Effectiveness of Intrathecal Chemotherapy
Clinical Success in CNS Cancer Treatment
Clinical studies report significant success of intrathecal chemotherapy in treating CNS cancers, improving survival and quality of life. This method’s ability to deliver high drug concentrations directly to tumors enhances its potency. Patients experience reduced neurological symptoms and longer remission periods. Ongoing research continues to refine intrathecal techniques, striving for better clinical outcomes and expanded therapeutic options for challenging cancer types.
Managing Adverse Reactions
Despite efficacy, intrathecal chemotherapy may cause adverse reactions such as nausea, headaches, or neurological symptoms. Oncologists carefully manage these effects through personalized care and supportive therapies. Regular monitoring and swift adjustments to treatment protocols help alleviate side effects. Ensuring patient comfort and safety remains paramount, with healthcare teams prioritizing side-effect mitigation alongside therapeutic success.
Conclusion
Intrathecal chemotherapy represents a pivotal advancement in CNS cancer treatment, offering targeted drug delivery with heightened precision and improved therapeutic outcomes. By utilizing the intrathecal route and bypassing the blood-brain barrier, this method enhances drug impact while reducing systemic exposure and associated side effects. Various administration techniques, from lumbar puncture to catheter-based systems, provide flexibility for individualized patient care. As clinical research progresses, this strategy continues to improve outcomes for those with complex CNS malignancies, reinforcing long-term hope in modern oncology.